Baby Rachel is officially one week old today! How is that possible?! I hate to sound like the stereotypical new parent but it really is amazing how much she has changed in just one week. Before I forget everything that happened one week ago, I want to share my birth story. Hopefully it will be encouraging or at least interesting to other moms to be (or just folks in general).
My birth story started, in my mind anyway, on Thanksgiving night. I worked that night & felt tired but decent. However, once I got home from work in the morning (on Black Friday) I started vomiting & generally feeling terrible. I just knew something wasn’t right. I texted my doula asking for advice & she recommended I call the midwife on call. I’m so glad I did because the midwife ended up asking me to come in to the hospital for a preeclampsia workup. By the time we made it to the hospital I had been up for 16 hrs straight or something ridiculous like that, but I knew I wouldn’t be able to rest until I knew what was happening to my body. As it turned out my BP was mildly elevated in the 130s/80s which isn’t too remarkable but higher than my baseline for the rest of the pregnancy. (At that point I was 37 weeks 4 days.) My labs also showed a slightly elevated protein to creatinine ratio but the midwife wasn’t acutely concerned. However, she instructed me to rest & to call the office first thing Monday morning so I could be seen that day instead of later in the week as previously scheduled. She also asked me to keep track of my BP over the weekend if possible.

Rachel ready to go home from the hospital
I felt reasonably well over the weekend but when I checked my BP at home it was consistently around 140/90. Granted this was me doing a manual BP on myself but I felt pretty confident my numbers were accurate, so first thing Monday morning I called for an appointment. When I went to the office a few hours later my BP was 142/88 & I had proteins in my urine, which was new for me. The midwife was hesitant to call it true preeclampsia yet but she did write me a note saying I could no longer work (that was supposed to be my last week of work anyway) & instructed me to come back for my regularly scheduled visit on Wednesday & to call any time with any symptoms or concerns.
The next morning, which marked exactly 38 weeks, I checked my BP at home & got 150/100. Naturally that was when I really started getting concerned. I decided to go to the grocery store & try one of the automatic BP machines at the pharmacy. That gave me a reading of 130s/80s but I just had a feeling it wasn’t very accurate. When I got home I spoke to the midwife on call, who turned out to be the same one I’d seen the day before, & she instructed me to recheck my BP in 4 hrs & then call back. However, after about an hour or so, she called me back & told me that after discussing my case with the doctor they felt the best plan was for me to come in to the hospital to be induced at 1:00 p.m. Part of me was scared but mostly I knew in my heart that this was the right plan.
I called my doula & she cautioned me that an induction at 38 weeks might be difficult & prolonged, but she also stated she would support me no matter what. The whole pregnancy I had been very committed to a natural birth, but I knew that with an induction I would almost certainly end up on Pitocin & that alone would greatly increase my “risk” of getting an epidural. But with her & my husband’s support I was determined to make the best of the situation. She encouraged me that she had survived not one or two but FOUR labors with Pitocin without an epidural or any pains meds. I also kept reminding myself that my mom survived an induction with Pitocin (due to hypertension) without an epidural or any pain meds. If they could do it, I figured I could too. Furthermore, I kept reminding myself that an induction due to preeclampsia, with a rather sudden onset no less, was not part of my original birth plan & that from everything I’d read the best way to have a satisfying birth experience is to keep an open mind & remain flexible while still staying true to your goals as much as possible. With that mindset I felt ready to go.

I swear she has so much personality already.
To make a long story short, the first afternoon/night in the hospital wasn’t very exciting. In the end that was probably for the best because it allowed me to get some decent rest to prepare for the big day that was to come. (My poor husband didn’t sleep a wink that night so I am eternally grateful to him for still managing to be the best labor support person ever despite his own exhaustion.) On arrival to the hospital my BP was 150s/90s. That was when I knew for sure we’d made the right decision in going forward with the induction. Unfortunately it took three tries for the nurses to get an IV in me, but I couldn’t be upset about that because I could look at my own hands & see how swollen they were. They also told me I had tough skin which I know from experience makes IV insertion much more challenging. Once they got the IV in place, they sent off labs & the midwife came in to check my cervix. To our great surprise I was already dilated 2 cm & 80% effaced. This was encouraging because it increased my chances of a successful induction. The midwife started me on Cytotec around 3:30 pm. We ended up doing another dose around 7:30 p.m. & a third dose around 11:30 p.m. (Cytotec helps “ripen” the cervix” & thus potentially start labor.)

After her sponge bath this morning
By 3:30 the next morning I was only dilated 3 cm & my contractions were not much stronger or more frequent, not enough to put me in true active labor anyway. The upside to that was I was comfortable enough to get some decent rest overnight, especially with the amazing sound machine (provided by the hospital) set to ocean waves. Around 4 am the midwife decided to try a fluid bolus to see if that would kick-start my labor. Unfortunately after 1L of IV fluids I still hadn’t really progressed. Yes, the dreaded P word was coming. I was “stuck” & needed Pitocin. But I was so ready to meet our baby girl that I said “screw it, throw it at me.” However, the nurse was kind enough to offer me a 1 hour break off the monitors to take a shower & eat a good breakfast. I’ll be eternally grateful to her for that because that made such a difference in how I felt once “real” labor began.
Just before 7 am the nurse came in to turn on the Pitocin. I was as ready as I was ever going to be. I’d kept the doula updated overnight & let her know that with the dreaded P on board I’d probably need her soon. Somewhere around 8 am my husband called her & told her we were ready for her support. That should be an indication that the pain had started to increase beyond mild cramps to something more intense. Over the next few hours things escalated pretty quickly. At first I was amazed at how much deep breathing helped relieve or at least distract me from the pain. However, eventually I started hitting a brick wall, so to speak. A lot of that time is a blur to me but Jared & the doula both have told me that between 10:00 & 11:00 were the roughest times. Believe it or not at that point the Pitocin was actually off because they were having so much trouble getting the monitors to read properly & I guess they figured they’d see how I did without it. To manage the painful contractions I tried multiple different positions/locations, including the birthing ball & the rocking chair & the tub, but none of them worked for too long. However, anything was better than just lying in bed. Plus I knew that the more I moved around the faster labor would progress. Somewhere around this time the midwife (a different one now) checked my cervix & I was dilated to 7 cm. That was really encouraging & helped me push through the next few painful hours. 
Eventually around 12:30 maybe I reached a point of utter exhaustion. I felt like I had used up all of my coping resources including deep groans, back massages, & position changes. I started crying & begging for an epidural or some kind of pain medicine. I even used my code word which my husband & I had set up with the doula ahead of time to indicate that I really truly wanted medicinal pain relief. The nurse & midwife were concerned I was too close to the pushing stage to safely receive either an epidural or narcotics but they needed to check my cervix to be sure. As it turned out I was dilated to 9.5 cm at that point & it was indeed too late. Part of me was massively disappointed while another part of me was like “Screw it, I’m almost there, I can do it!” Everyone kept telling me the urge to push would be undeniable but to be honest it really wasn’t at first. But it wasn’t long before the midwife told me my cervix was fully dilated & effaced & it was pushing time. My doula kept reminding me to bear down during the pushing to help relieve the pain & make my pushes more effective. As physically challenging as pushing was, it was actually not as painful as the previous few hours of contractions. Unfortunately after an hour or so of pushing my body was simply wearing out & my uterus wasn’t contracting hard enough to match my pushes. The midwife wanted to turn the Pitocin back on because we could see the baby’s head but I just couldn’t seem to progress (thank goodness for the big mirror because it really encouraged me to see how close she was when I was so ready to admit defeat). I was scared to death to get the Pitocin back but I also knew that anything that brought me closer to the finish line faster was worth it so I said yes. It was at that point that I realized my IV appeared to be coming out of my wrist. I thought I was going to die when I saw that. Thank goodness the nurses were able to save it & restart the Pitocin, & within a few minutes baby Rachel made her grand entrance at 2:35 p.m.

I totally understand the term baby burrito now.
I’m not going to lie, in those first few moments I wasn’t as overwhelmed with that immediate love spell as I had hoped I would be. As they placed her on my chest I was mainly just thankful that labor was over. My mind was mostly focused on being grateful for an end to the pain & exhaustion. I had read that this is fairly common so I knew not to judge myself too harshly & that soon enough the overwhelming feelings of love would wash over me. As it turned out my placenta took a while to deliver. The midwife kept the Pitocin on because once again my contractions just weren’t strong enough on their own to push it out. Once the placenta finally delivered, the midwife & the nurses were astonished to discover that it had an extra lobe. They told me this was extremely rare & asked to take pictures of it. Being a nurse of course I said yes, as I was equally fascinated by this odd turn of events.

This was about 1.5 hrs post delivery. Pretty sure this child came out sucking her thumb.
While we waited for the placenta to deliver, my husband cut the cord (we opted for delayed clamping of about 3-5 minutes which is actually standard practice with my group of midwives). Next my husband held her on his bare chest for skin to skin care which was when I realized how much I truly love this man. Then the charge nurse & another nurse took Rachel to the bassinet across the room to do her Vitamin K injection & newborn assessments. The nursery nurse soon came & thankfully recognized that Rachel was acting a bit more jittery than average & thought to check her blood sugar. When she announced it was 34, I almost yelled “Holy shit, get the D50!” Thankfully as the nurse explained a newborn’s blood sugar only needs to be about 40 to be normal so it wasn’t actually that low (whereas a blood sugar of 34 in an adult is definitely a medical emergency). At that point the nurse handed Rachel back to me, & the doula started helping me try to breastfeed. Unfortunately Rachel was too jittery to really concentrate & I was too exhausted both mentally & physically to have a clue what to do. The nursery nurse ended up giving her a small bottle of formula to raise her blood sugar & thankfully that was successful. 
Sometime while all of this was happening, the placenta actually delivered & the midwife assessed me for the need for stitches. As it turned out I was very blessed & only had a very small internal laceration requiring just two or three stitches. By that point the oxytocin love bath had begun so I seriously didn’t even feel the lidocaine injection they gave me to numb me before the stitches.
To make a long story short, over the next 12 hrs or so the nurses had to check Rachel’s blood sugar every few hours. Unfortunately it did drop once & she had to receive another small dose of formula around 8 pm to stabilize her. After that her blood sugar was never a problem again. However, her bilirubin became an issue but was consistently just below the borderline of needing treatment. We were discharged on Friday with an appointment to follow up with our pediatrician the very next morning. My parents left Friday morning & that night at home was very rough. I was breastfeeding Rachel every one to two hours but she was so lethargic that I could never be sure she was actually getting anything out of of it. She also went from having tons of dirty/wet diapers in the hospital to having very few at home. At some points she was inconsolably crying & in my heart I just knew something was wrong. If we hadn’t had the appointment at 10 am on Saturday I probably would have taken her back to the hospital.
When we went to the appointment on Saturday the doctor was extremely friendly & knowledgeable but she didn’t dance around the truth. She told us Rachel was definitely jaundiced & had a high risk of needing bili light therapy to reduce her bilirubin. She taught me how to use my breast pump (there’s a reason I chose a pediatrician who is also a lactation consultant . . . & whose office is 3 minutes from our house) & instructed me to feed Rachel at least 30 mL every 2 hrs & to supplement with formula (which she gave me) if needed in order to achieve that goal. As soon as we left the office we headed across town to have her bilirubin rechecked. Because it was a weekend they couldn’t do it in the office & get fast results but one of the local hospitals could. The doctor promised to call us within a few hours with the result. As it turned out we had just made it home from the hospital lab & I was pumping when the doctor called Jared to say Rachel’s bilirubin was too high & we needed to take her to yet another hospital for one to two nights of bili light therapy.
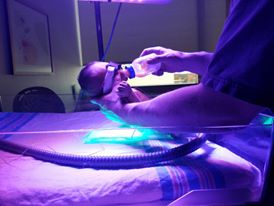
My husband feeding Rachel under the bili light
Immediately I dissolved into tears. Part of me was so thankful to know that my “mama instinct” was right & that Rachel’s behavior wasn’t normal, but of course the other part of me was scared to death. We ran around getting our bags repacked, managed to forget one of them, & raced off to the hospital, which happened to be the one hospital in Raleigh that I had never actually laid eyes on in the four years we’ve lived here. When we arrived at the hospital, I was pleased to see that they were expecting us at patient registration & got us up to a very nice room within about 30 minutes. Not long after that the bili light was started. My parents came back that night after I called my mom in tears & told her I needed her. I will forever be grateful for their unwavering support during such a difficult time. Overnight my milk came in, & this, coupled with the bili light, was exactly what Rachel needed to get better quickly. We ended up staying just that one night & were discharged the next day, which happened to be my 28th birthday, less than 24 hrs after our admission. Seeing our baby girl doing so much better was the best birthday gift ever. I have tears in my eyes just thinking about it now.

Now this is what you call a milk drunk baby.
First thing Monday morning my husband called the pediatrician to see when she wanted us to follow up with her. Based on the information she received from the hospital she said we could wait until the next morning. During our visit yesterday the pediatrician gave us a great report & was very pleasantly surprised to see that Rachel had gained 8 oz just since Saturday. She said I no longer needed to worry about knowing exactly how many mL Rachel was consuming with each feeding, so she spent a great deal of time helping me breastfeed effectively. Not long after we got home from that appointment, the lactation consultant from our doula group came over for a consultation. Let me just say that was the best $150 ever spent. By the time she left our house I felt super confident in my ability to breastfeed Rachel & no longer felt reliant on the pump. It’s been over 24 hs now & I haven’t needed to pump at all other than to relieve some mild engorgement. My milk might have been a little slow to arrive but now that it’s here I have an abundance! Being able to breastfeed effectively has greatly increased my mommy confidence. Additionally Rachel & I both slept so much better last night because she has had far less gas issues & hiccups now that she’s off the bottle. Amazing!

This might be my favorite picture ever, so I’ll share it again.
Well, that is my long, somewhat complicated but also very fulfilling birth story. We definitely hit a few speed bumps along the way but nonetheless I truly feel like I had the most fulfilling birth for which I could have hoped. The best part of the process of course was the ultimate outcome of our beautiful baby girl. But the second best part is the amazing confidence boost I’ve gained from surviving an unmedicated induction. Part of the reason I was so determined to have an unmedicated birth was because I knew that for the rest of my life I’d be able to tell myself “I survived that so whatever else life throws at me, I’ve got this.” Thankfully that prediction came true & I am feeling more confident than ever. Not to mention in love with the cutest baby ever!
In my next post I’ll be sharing my tips for why I believe my pregnancy, birth, & initial postpartum period went/have gone so smoothly. This first week of motherhood has been a wild & crazy ride, but it’s without a doubt my favorite journey ever.



