Last Fall I wrote a post entitled The New Grad Nurse’s Survival Guide which has since become one of my most popular posts to date. That post includes tips to help new nurses acclimate to the fascinating but often challenging & frustrating world of hospital nursing. Today I thought it would be beneficial to create a survival guide for those nurses, like me, who struggle with anxiety issues. You will notice a lot of overlap between the two posts, but nevertheless I hope that you will find this post helpful if you too struggle with anxiety both in your personal life & as a nurse.
Disclaimer (because we live in a wildly litigious society these days): As you read this post, keep in mind that I have no official psychiatric credentials. This list is based purely on MY OWN PERSONAL EXPERIENCE & is in no way meant to diagnose, treat, or cure any condition.

I struggle with anxiety, but I’ve found that this blog is a great way to tame the “anxiety monster.”
- My first recommendation is to get to work as early as you’re allowed to clock in so that you can maximize the amount of time you have to read up on your patients before receiving report. This will allow you to already have a basic idea of what is going on with your patients & thus empower you to ask good questions in report.
- After finishing report, take time to look up more information on your patients before you start seeing them (provided no one has an urgent need of course). I’ve found that the more background information (labs, test results, etc) that I have on my patients, the better I feel about taking care of them. This came into play recently when I had a patient who ended up in ICU not long after the start of my shift. If I hadn’t taken the time to write down the patient’s history, labs, etc at the beginning of my shift, I would have been scrambling to look up that information during a very emergent situation . . . which is obviously less than ideal. I’ve found that my anxiety is much better controlled if I start out my shift knowing as much as possible about my patients because I know that if an emergency occurs, I’ve already got my head in the game, so to speak.
- To be clear, I try, at minimum, to glance through all the current orders, the H&P, the most recent lab/test results & vital signs, & the most recent doctor’s note(s) on each patient before starting my rounds. Obviously this doesn’t ALWAYS happen, but I make it a priority to have it done ASAP no matter what because I’ve found it does help me so immensely.
- On a similar topic, find or create a good report sheet that will help you stay organized. After several tries, this is the one I’ve come up with that I’ve found works best for me. Feel free to use it or adjust it to make it work better for you. DO NOT FEEL LIKE YOU HAVE TO WRITE EVERYTHING FOR EVERY PATIENT ON ONE PAGE! I did that as a new grad, & I look back & want to slap myself because it only made me more anxious than I would have been if I’d just used a separate page for each person (duh!).

- Review all lines, drips, wounds, etc during report (preferably at the bedside). This way you can ask the off-going nurse about any discrepancies you find. Doing so is an easy way to help prevent errors, so don’t skip this simple but important step which can save you a lot of anxiety later in your shift.
- Stock your pockets with the most commonly used items at the beginning of your shift (before or after report) & periodically throughout the shift as needed. The things I always carry are alcohol swabs, blue caps (for IV lines), saline flushes, my scissors & penlight, a pen & a highlighter, & a roll of tape. I’m borderline OCD, so I’ve quickly learned that I feel naked without any of these things in my pockets. I’ve also found that my shift flows a lot more smoothly when I carry these things around because I’m not constantly running up & down the halls for something as small as an alcohol swab. Wasting time on little things that like, for me anyway, creates a lot of unnecessary anxiety that can be easily avoided by simply stocking my pockets on a regular basis.

- Establish some kind of routine & stick to it as much as possible. You can read about my routine here under #6.
- Following closely on the heels of the above point, learn to group tasks as much as possible. On my unit we as nurses take our own vital signs, & I’ve learned that the vast majority of the time it is more efficient for me to do vital signs, assess, & medicate each patient before I move on to the next one, rather than doing vital signs & assessments on every patient & then going back to do meds on each one. Do I have to break this practice sometimes when one patient has an urgent need or I get an admission at the beginning of the shift? Of course. But the point is that I’m making good use of my time rather than running in & out of my rooms constantly. Does this sometimes mean I’m a little later seeing my last patient? Sure. But as long as I know that patient is stable, I don’t think that’s a big deal because I feel like I’m able to devote more time to each patient as I go along rather than constantly being rushed between rooms. If your routine is different than mine, that’s ok. JUST FIND WHAT WORKS FOR YOU!

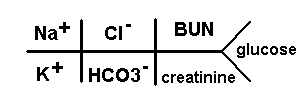
- Write down your meds/tasks & the times associated with each, & scratch them off or highlight them as you complete them. For me doing this not only organizes my shift but also gives me a great sense of accomplishment as I highlight the meds & tasks I’ve accomplished. I also write in important labs so that I don’t forget to check for those (e.g. coags on a patient with a heparin drip, Troponins on a chest pain patient, etc).

- Don’t be afraid to ask for help when you start to feel overwhelmed, & be specific in your requests for assistance. I’ve found that people are a lot more likely to actually help me when I’m specific in my requests. For example, if I know I have an admission coming but one of my other patients is unstable, I’m going to say something like this to the charge nurse, “Hey, as you know I’ve got this admission coming to room 5, but room 10 is having a lot of trouble breathing right now. I’m going to need you get vital signs on the new patient & get them settled so that I can take care of this situation in 10.”
- On the converse, if you see someone else who is struggling, don’t just say “Do you need help?” Of course they need help! Be specific in your offer to help them. For example, “I know you’re really busy right now. Whose meds can I give for you?” Or “I know your new admission is really sick & I heard you say he needs a new IV site. I’ll go try to get a new IV on him.”

- On the converse, if you see someone else who is struggling, don’t just say “Do you need help?” Of course they need help! Be specific in your offer to help them. For example, “I know you’re really busy right now. Whose meds can I give for you?” Or “I know your new admission is really sick & I heard you say he needs a new IV site. I’ll go try to get a new IV on him.”
- Celebrate your strengths & recognize your weaknesses. Being a nurse who struggles with anxiety is definitely a challenge at times. This job is difficult enough without being a perfectionist; trust me I know! However, I also know that my meticulous nature is a great part of what makes me a good nurse. I could describe dozens of situations in which I’ve made a significant difference in a patient’s life because of how obsessively I’ve watched their labs, respiratory status, vital signs, etc. However, I also know that because of my “sensitive” nature, I’m prone to burn-out, & thus I can’t work much OT without feeling like I want to quit my job &/or lose my mind. I recognize this & thus I don’t work much OT because I know it’s not in my best interests psychologically. I’ve also had to learn (& believe me it’s a continual learning curve) that it’s ok to not know everything or be perfect at everything all the time. No one is THAT good.

- On a similar note, find ways to manage your anxiety outside of work. I’ve found that seeing a therapist about once a month is a HUGE benefit to me. I can’t tell you how much I wish I had started therapy years ago, before I even became a nurse. Yes, friends & family are great, but there is something very unique about having an objective person who can listen to your struggles (both as a nurse & outside of work) & help you recognize methods to better manage your anxiety. Going hand in hand with therapy, don’t be afraid to take medications for your anxiety if your medical provider recommends it (& don’t be afraid to ask for meds if you feel like that is needed). I was very hesitant to take any psychiatric meds, but I started taking Prozac last summer, & there are no words to describe how much better I feel these days. No, it’s not a magic “happy pill,” but I have found that it “takes the edge off” so to speaks & thus helps me to stay calm & better able to survive anxiety-provoking situations, whether at work or at home. TAKING MEDICATION FOR ANXIETY IS NOT A WEAKNESS. I still have to tell myself that sometimes, but the point is that I’m better able to function as a nurse, a wife, a friend, a daughter, a dog mommy, & just as a human being thanks to Prozac. If that’s not a good enough reason to take a medication, I don’t know what is. In addition to therapy & Prozac, I’ve also found that writing (hello, blog!), music, & exercise are great sources of stress relief for me, so making time for those is extremely important. It is true what they told you in nursing school: YOU CANNOT TAKE CARE OF OTHERS IF YOU DON’T FIRST TAKE CARE OF YOURSELF. Don’t forget that!

Fellow nurses, feel free to comment with any suggestions you have for how to navigate the healthcare world, as chaotic as it often is, while living with an anxiety condition. It is definitely not easy, but it CAN be done. Trust me, I still have shifts where I have to step into the break-room for a minute just to clear my head (or occasionally to wipe the tears of frustration from my eyes), but I’ve found that those times are much fewer now that I follow the tips outlined above. As I stated at the beginning, these are just the things that I’ve found work for ME, but I’d like to believe they could be helpful to others as well.
I’ve said it before & I’ll say it again: learning to live with anxiety is a continual learning process. Some days are better than others, & that’s the way it will always be. We just have to learn not to let the bad days get us down forever. We must keep fighting the good fight because as nurses our patients desperately need us.